April happens to be Adenomyosis Awareness Month. I couldn’t very well let that slide by without having a conversation about adenomyosis, endo’s twin sister! There is a high percentage of people with endometriosis who also have adenomyosis and vice versa. Today we are going to explore adenomyosis, including what it is, what the common symptoms are, and how it is diagnosed. In particular, we will explore the question I get asked most frequently, which is, “what is the difference between endometriosis and adenomyosis?”
So what is the difference between endometriosis and adenomyosis?
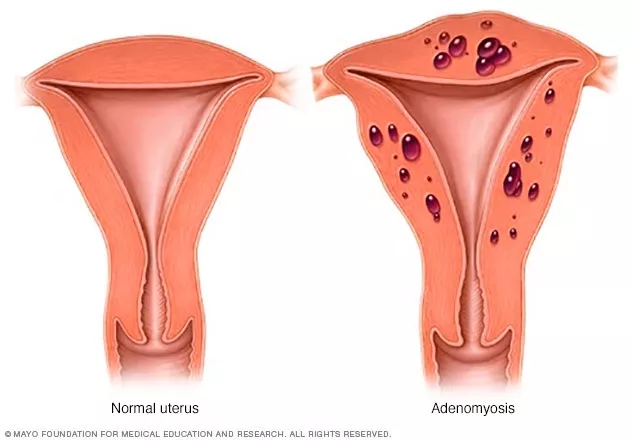
Endometriosis is a condition in which tissue that is similar to the endometrial lining of your uterus grows outside of your uterus. With adenomyosis, this tissue grows instead inside of the muscular wall of the uterus.
Symptoms of adenomyosis include an enlarged uterus, inflammation of the uterus, heavy and painful periods, pain with sex, pelvic pain, and feelings of abdominal bloating, fullness or heaviness.
Many of the symptoms of endometriosis and adenomyosis overlap, so if some of these symptoms sound familiar to you that is probably why!
How is adenomyosis diagnosed?
There is also a difference between endometriosis and adenomyosis in the way that they are diagnosed. Unfortunately, both conditions require surgery to be definitively diagnosed.
Certain signs might tell your doctor to suspect adenomyosis. This can include your symptoms and a pelvic exam, or even imaging like an ultrasound or an MRI. These options can’t give you a definitive diagnosis though, only suspected adenomyosis.
Endometriosis can be diagnosed via a laparoscopic surgery where endo lesions can be seen as well as removed. Adenomyosis is a bit more difficult with the tissue being inside of the uterine wall. The only way to truly diagnose it is to have a hysterectomy and have the tissue checked out after the fact.
Now of course having a hysterectomy just isn’t an option for everyone. For a woman who is young and may still want to have children, having your uterus removed will not be a great option. Even for a woman who is already perimenopausal or menopausal, removing an organ is something that should be heavily considered and not taken lightly.
Hysterectomy absolutely might be the right option for some women. My best recommendation is to do your homework, ask all the questions, and make sure it is the best option for your unique situation. In other words, make a fully informed decision!
I’ll take this moment to remind us all again that while hysterectomy can treat adenomyosis, it cannot treat endometriosis. With endometriosis, the tissue grows outside of your uterus so unfortunately removing your uterus will not prevent further progression of endo, even though you will stop having periods. Many women with endo have hysterectomies and still end up having endo symptoms again further down the line!
What is the difference between endometriosis and adenomyosis treatment?
We already talked a bit about the different surgical options for endometriosis and adenomyosis. If that is something you are considering, I highly recommend connecting with a surgeon who specializes in this area, like those you can find on Nancy’s Nook.
In the world of Western medicine, there are a few other non-surgical options that are commonly used to treat both endometriosis and adenomyosis. These include hormonal treatments like birth control or other hormone-blocking medications as well as anti-inflammatory medications.
In the effort to help women to make fully informed decisions, it is so important to know that all of these medications come with side effects. Birth control has a huge number of known side effects, ranging from headaches and mood changes to suicidal thoughts. It also causes a huge amount of nutrient depletion, which is something that should be considered for anyone who is on birth control.
There is a wonderful documentary called The Business of Birth Control that does an excellent job of exploring this side of birth control that no one really talks about.
Now of course the decision of whether or not to go on birth control or other medications should be made between you and your doctor. It may end up being the best decision for you. But please, again, do your research, ask questions, and make a fully informed decision for yourself.
How can you approach adenomyosis holistically?
I’m so glad you asked! Looking at medical treatment options alone can sometimes feel overwhelming, confusing, and disempowering. The truth is though that there is so much you can do to support your body naturally as well.
Both endometriosis and adenomyosis can progress over time, but they also can stabilize or even regress. There have been studies on this, although they are not always talked about in the medical world.
Just speaking for myself and my own experience, I know that I have endometriosis based on my laparoscopic surgery. I have suspected adenomyosis, based on what my surgeon observed in seeing my uterus during surgery. Since I personally do not plan on having a hysterectomy ever if I can help it, I likely will never know definitively.
What I can do is look at how my symptoms have changed over time. My periods have gone from being agonizingly painful to basically pain-free, I no longer have any pain with sex, and feelings of abdominal discomfort have gone down immensely.
A big part of this has been addressing my gut health, inflammation, and stress. Let’s take a quick peek at what that looks like!
What is the difference between endometriosis and adenomyosis as far as how you eat and care for yourself?
The great news here is that the things you do to care for yourself for one also help with the other! Endometriosis and adenomyosis both have a strong root in immune dysfunction and inflammation, so addressing those things can have a major impact on both.
One of the major influences here is what you put in your body. Focusing on eating real, whole foods and avoiding foods that contribute to inflammation like processed foods, vegetable oils, sugar, and alcohol can make huge impacts in and of itself.
Others strategies I have used for myself as well as my clients in my practice include addressing gut health by taking a close look at digestive health, imbalances in your gut, and food sensitivities. Stress management is a huge piece of the puzzle as well, along with being intentional about how you are moving your body.
I have several posts I have written about these topics in more depth in the past, so I will link to those below in case you would like to know more about how this works.
Where to begin if you have endometriosis or adenomyosis
Receiving a diagnosis, suspected or confirmed, of endometriosis or adenomyosis can feel overwhelming. My best advice is to take it one day at a time. Make one small change for the healthier today and then keep at it, little by little.
My other best advice is to build a support team around you. Don’t try to go it all alone. Find a quality doctor who specializes in this area and look into various practitioners who can support you holistically, including nutrition and gut health, possibly pelvic floor therapy, massage, acupuncture, and more. There are so many incredible professionals out there who are happy to help you on your journey.
Is this all an investment? YES! But your health is everything. If there is just one area in your life where you splurge a little, let it be this. Your body will thank you!
So much love to you on your journey, my friend! If you are ready to take the next step in your journey towards health and healing, I would love to be a part of that journey with you. Click here to learn more about my Thrive With Endo program and apply today!
Other Articles You Might Enjoy:
Endometriosis and Gluten: What You Need to Know
The 5 BEST Foods for Endometriosis
The 5 WORST Foods for Endometriosis
Elimination Diet for Endometriosis
Resources:
References:
Taran, F.A.; Stewart, E.A.; Brucker, S. (2013). Adenomyosis: Epidemiology, Risk Factors, Clinical Phenotype, and Surgical and Interventional Alternatives to Hysterectomy. Retrieved from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3859152/
Chernofsky, Mildred R, MD. Adenomyosis. Retrieved from: https://www.hopkinsmedicine.org/health/conditions-and-diseases/adenomyosis#:~:text=Adenomyosis%20(pronounced%20add%2Den%2D,to%20very%20heavy%20menstrual%20bleeding.
Romm, Aviva. (2017). Pill: Are the Risks Too Bitter to Swallow? Retrieved from: https://avivaromm.com/the-pill-risks/
Palmery, M., Saraceno, A., Vaiarelli, A., Carlomagno, G. (2013). Oral contraceptives and changes in nutritional requirements. Retrieved from: https://pubmed.ncbi.nlm.nih.gov/23852908/
Mayo Clinic. (2018). Endometriosis. Retrieved from: https://www.mayoclinic.org/diseases-conditions/endometriosis/symptoms-causes/syc-20354656


